What Happens After a Hip Arthroplasty (Replacement)?
Know what to expect, and when and how to best help your loved one immediately following a hip replacement.
Get insurance benefits, legal documents, and medical records in one place
Helpful Highlights
There are a few do's and don'ts with a freshly replaced hip joint.
Observe for post-surgical complications and report them to the surgeon, as well as the primary care provider.
Encourage your loved one to commit to physical therapy for the best chance of success.
Walking is the best thing your loved one can do to get stronger after hip replacement. Encourage them to walk with you.
After hip arthroplasty (replacement)
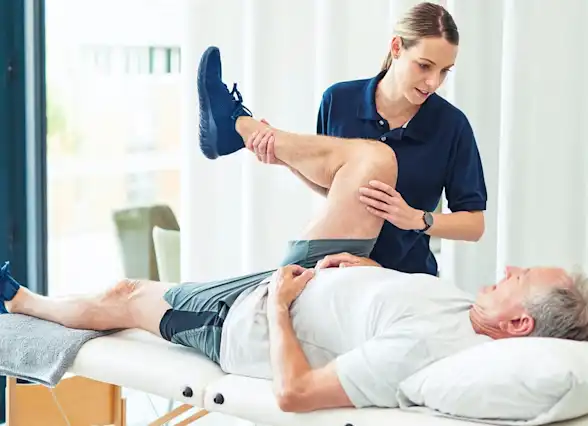
Hip replacement recovery starts right away. Your loved one will be encouraged to get up and move around as soon as possible after surgery. People who don’t have complicated health conditions can go home as soon as they demonstrate that they can walk, climb stairs, and get in and out of a car.
To accomplish these tasks, your loved one might spend time in an inpatient rehabilitation unit. Whether they go home or to a rehabilitation unit after surgery, they will need physical therapy for several weeks until they regain muscle strength and appropriate range of motion.
The surgeon will discuss rehabilitation needs, what to expect in the days and weeks ahead, and how to make the most of recovery. Your loved one's motivation and cooperation in completing the physical therapy is critical for an effective recovery process and overall success of the surgery, and as their caregiver, you play an integral role in that.
Post-surgical complications are not uncommon and can be managed when caught and reported early. Let the surgeon’s office know right away if you or your loved one notice:
Shortness of breath.
Chest pain.
Increased redness or warmth around the surgery site.
Painful swelling or increased drainage from the incision (regardless of color), or foul odor.
High fever (greater than 102 degrees F), or temperature below their normal.
Shaking chills.
Sudden, severe pain in the joint.
New pain in the calf, ankle, or foot, or swollen and tender calf that causes pain when walking.
If pain is not improving as expected or instructed.
Physical therapy
After joint arthroplasty (replacement), there are some good guidelines to follow regarding acceptable physical activities. Activities should NOT...
Cause pain, including pain felt later.
Jar or impact the joint.
Place the joint in extreme ranges of motion.
Most people use a walker or crutches for up to a month following hip replacement surgery, and then a cane for a couple weeks beyond that.
Daily activity and exercise can help your loved one regain the use of their joints and muscles. A physical therapist will teach strengthening and mobility exercises to do at home and will help your loved one learn how to use a walking aid. As therapy progresses, they will gradually increase the amount of weight they put on their leg until they're able to walk without assistance. They should expect to do 10-15 minutes of exercise several times a day, every day, for about two months following the operation, but the best exercise for a hip replacement is simply walking.
You can encourage them to get the exercise they need by offering to do their exercises with them and inviting them to go on walks.
The length of physical therapy varies based on age, fitness, and level of motivation but usually lasts for about 6 to 8 weeks. Two to three therapy sessions per week are average for this procedure.
Results
Full recovery from hip arthroplasty (replacement) varies from person to person, but most people are doing well three months after the surgery. Improvements typically continue during the first year after surgery.
Joint replacement success will strongly depend on how well your loved one follows the orthopedic surgeon’s instructions. As time passes, they should experience a dramatic reduction in joint pain and a significant improvement in their ability to participate in daily activities. Remember, however, that joint replacement surgery usually does not result in the ability to do more than they could before developing joint problems.
Reiterating this expectation for yourself and your loved one is important.
Long-term limitations
The goal of total hip arthroplasty (replacement) is to return to a high level of function without hip pain and a large majority of people can achieve this goal; however, limitations apply. Here are some common-sense guidelines for your loved one's active lifestyle.
Recommended:
Walking (flat ground, good shoes)
Swimming (avoiding breaststroke kick)
Water aerobics
Cross-country skiing
Cycling or stationary bike
Elliptical machine
Golf
Dancing (more ballroom style, not swing or hip-hop)
Office work versus fieldwork
Permitted:
Hiking
Slow speed stair stepping machine
Rowing
Gentle doubles tennis
Gentle downhill skiing (think bunny hills, no steep faces, and no moguls)
Light labor (jobs that involve driving, walking, or standing, but not traversing uneven ground or heavy lifting)
Prohibited:
Jogging or running (including on a treadmill)
Heavy weightlifting
High-impact exercises - those with hard stops/starts and jumps (squash, racquetball, volleyball)
Sports that require constant or extreme twisting/pivoting (singles tennis, basketball)
Contact sports (football, wrestling, martial arts)
Heavy labor
Talk to your loved one's surgeon and primary care provider about activity permissions and restrictions specific to their case.
RESOURCES
American Academy of Orthopaedic Surgeons (AAOS) – Total Hip Replacement
American Association of Hip & Knee Surgeons (AAHKS) – Total Hip Replacement
Johns Hopkins Medicine – Hip Replacement Surgery
No content in this app, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.
Get more support and guidance on insurance benefits, medical records and legal forms.
Helpful brings together your insurance benefits, legal documents, and medical records in one personalized place — so you always know what you have, and never have to search again.
Technology for Health Tasks. Mental Health for the Tough Stuff.
Helpful connects your medical records, insurance, and caregiving tasks automatically. And when you need more than logistics, a therapist is here to guide you.
In-Network and Covered
For Individuals, Couples and Families
HIPAA Compliant, Data Stays Private

Healthcare Tasks Simplified

From syncing records to spotting drug interactions, Helpful does the heavy lifting, turning complex health info into clear tasks and showing you benefits you can actually use, giving you clarity and control over your care.

In-Network Mental Health

Our licensed therapists are here to support you and your loved ones through stress, burnout, and life’s hardest moments, with an inclusive, compassionate approach that works with most insurance plans.

Create Legal Documents

Plan ahead by creating will, trusts, advance directives and more, that ensure your wishes are honored in the event you can’t speak for yourself -with Helpful guiding you every step of the way.