What Do I Need to Know About Hip Arthroplasty (Replacement)?
Hip arthroplasty is the same thing as hip replacement. Surgeons expect more than 50% of hip replacements to last about 25 years.
Get insurance benefits, legal documents, and medical records in one place
Helpful Highlights
Arthroplasty is the medical term for joint replacement surgery.
There are three surgical approaches to hip replacement: posterior, lateral, and anterior. Posterior is most common and lateral is not often used.
Surgery is often minimally invasive, though there are cases that require traditional open surgery.
As with any surgery involving general anesthesia, it is important to exercise the lungs frequently over the following few days.
Some medical professionals use the term hip “arthroplasty,” while others use hip “replacement.” However, the terms are interchangeable. Likewise, you may also hear or see them abbreviated as THA or PHA (total or partial hip arthroplasty).
The surgical approach
The surgical approach depends on several factors, including how the surgeon will gain access to the hip, the type and style of the implant and how it will be attached, your loved one's age and activity level, and the shape and health of the hip. The likelihood of future surgery also figures into the decision, because some surgical approaches and implant attachments can make a revision surgery easier or more challenging.
As part of the evaluation for surgery, the orthopedic surgeon will explain how they plan to perform the surgery (minimally invasive or traditional open), as well as what type of implant and attachment method will be used.
There are three surgical approaches for performing hip arthroplasty (replacement). Each of these approaches can be minimally invasive or traditionally open.
The posterior approach (also referred to as "muscle-sparing") is the most common, where the surgery is performed from the back of the hip joint.
The lateral approach is where the surgery is performed from the side of the hip joint.
The anterior approach (sometimes "mini", "modified", or "direct") is where the surgery is performed from the front of the hip joint.
Minimally invasive versus traditional open surgery
Minimally invasive hip arthroplasty (replacement) aims to minimize the impact of surgery on healthy tissues, such as muscles and blood vessels. When the surgery is minimally invasive, the surgeon accesses the hip joint through one or two small incisions (generally no more than 3 inches) by moving the muscles aside. This approach may have advantages, such as:
Lower risk of muscle damage
Less pain
Quicker and easier recovery
Less limping
Shorter hospital stay
Lower chance of hip dislocation
Minimally invasive hip replacement is not appropriate for all persons, however. In that case, traditional open surgery must be performed, where skin layers are cut and folded back and muscles must be cut through to access and replace the hip joint. Sometimes minimally invasive surgeries become traditional open surgeries if the orthopedic surgeon encounters barriers to minimally invasive surgery once in the surgical suite.
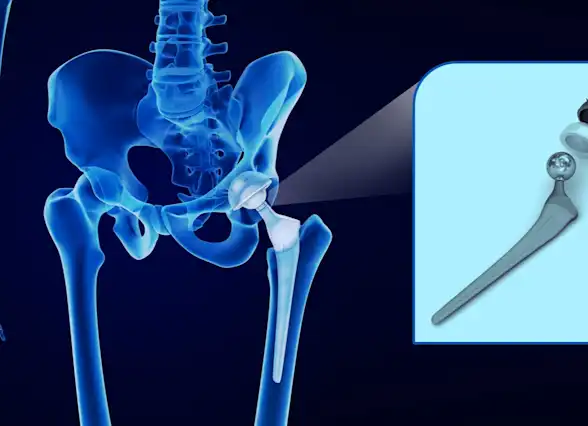
Parts of a hip implant (prosthesis)
The hip replacement implant, also called hip prosthesis, has two parts:
A ceramic or metal alloy ball is attached to a short metal stem, which is inserted into the top of the thigh bone (femur, femoral head).
A metal alloy cup with a durable, medical-grade plastic layer, which is attached to the pelvic socket of the hip joint (acetabulum) allows the ball implant to rotate smoothly - just like a natural hip joint.
Note that in a partial hip replacement, only the femoral head implant is used.
Overview of hip arthroplasty (replacement)
A single total hip replacement is typically completed within 2-3 hours (partial hip replacement may be shorter and double hip replacement will be longer). To perform a hip replacement, the orthopedic surgeon:
Makes an incision over the hip, through the layers of tissue.
Removes diseased and damaged bone and cartilage, leaving healthy bone intact.
Implants the metal replacement socket into the pelvic bone.
Inserts the ceramic or metal ball and stem into the top of the thigh bone.
Secures the implants either with bone cement, or an advanced material used to promote bone regrowth.
May get x-rays or other imaging following the procedure to ensure proper alignment and a successful joint union.
Can both hips be replaced at the same time?
Both hips can be replaced during a single surgery. A double hip replacement is also called a bilateral hip replacement. If your loved one is having issues with both hips, the surgeon may recommend a double hip replacement, provided your loved one is in generally good health and can tolerate a longer surgery and a more challenging recovery.
Revision hip arthroplasty
While orthopedic surgeons anticipate that more than 50% of hip replacements will last 25 years, hip implants do wear out or loosen over time. It might also become damaged if your loved one suffers an injury or dislocation of the replaced hip. Once that occurs, revision surgery may be needed to replace the damaged parts of the prosthesis. Your loved one can extend the life of their implant by stretching, doing regular low-impact exercises (walking, golf, cycling, yoga, tai chi, swimming - avoiding breaststroke kicks), avoiding high-impact exercise (such as jogging, leg presses), and taking precautions to avoid falls.
With partial hip replacements (the femoral head only), a revision may be needed down the road to replace the socket (acetabulum), as well.
After the procedure
After surgery, your loved one will be moved to a recovery area (commonly called PACU - post-anesthesia care unit) for a few hours while the general anesthesia wears off. Medical staff will monitor their blood pressure, breathing, pulse, alertness, pain or comfort level, and need for medications. Any potential problems are immediately reported to the anesthesiologist (generally not the orthopedic surgeon, as anesthesia is the expert in post-surgical recovery).
Once admitted to a medical-surgical unit in the hospital or discharged home, your loved one will be asked to - frequently - breathe deeply, cough, or inhale and exhale using a device that keeps fluid out of the lungs (known as an incentive spirometer and a breathing trainer). How long your loved one stays in the hospital after surgery depends on their individual needs, though many people can go home the same day as surgery.
For more on what to expect when your loved one goes home, see content on Preparing to Return Home After Hip Replacement and What Happens After a Hip Replacement?
RESOURCES
American Academy of Orthopaedic Surgeons (AAOS) – Total Hip Replacement
American Association of Hip & Knee Surgeons (AAHKS) – Total Hip Replacement
Johns Hopkins Medicine – Hip Replacement Surgery
No content in this app, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.
Get more support and guidance on insurance benefits, medical records and legal forms.
Helpful brings together your insurance benefits, legal documents, and medical records in one personalized place — so you always know what you have, and never have to search again.
Technology for Health Tasks. Mental Health for the Tough Stuff.
Helpful connects your medical records, insurance, and caregiving tasks automatically. And when you need more than logistics, a therapist is here to guide you.
In-Network and Covered
For Individuals, Couples and Families
HIPAA Compliant, Data Stays Private

Healthcare Tasks Simplified

From syncing records to spotting drug interactions, Helpful does the heavy lifting, turning complex health info into clear tasks and showing you benefits you can actually use, giving you clarity and control over your care.

In-Network Mental Health

Our licensed therapists are here to support you and your loved ones through stress, burnout, and life’s hardest moments, with an inclusive, compassionate approach that works with most insurance plans.

Create Legal Documents

Plan ahead by creating will, trusts, advance directives and more, that ensure your wishes are honored in the event you can’t speak for yourself -with Helpful guiding you every step of the way.