Distinguishing Diabetes Distress, Diabetes Burnout, and Depression
Diabetes distress and burnout are real and they are distinct from each other. They are also wholly different from depression.
Get insurance benefits, legal documents, and medical records in one place

Helpful Highlights
Diabetes distress is different from - but can lead to - diabetes burnout.
Depression is wholly separate from both conditions and may or may not also be present.
Proper care planning depends on distinguishing the conditions present.
Your loved one, especially after years of living with diabetes, may experience distress or burnout. The signs and symptoms of distress and burnout may not be obvious or they may look like depression. However, they are very distinct from one another, and the presence of distress or burnout does not necessarily mean there is depression.
Both make it more difficult for your loved one to manage their diabetes and maintain adequate self-care. To provide appropriate and personalized treatment, providers should make the clinical distinction between distress, burnout, and depression before planning care. If you have concerns about any of these conditions, accompany your loved one to an appointment with their provider to discuss what you're seeing, and consider seeking support from a mental health provider.
What is diabetes distress?
Managing diabetes involves significant effort by your loved one every day, every week, every month, every year, year after year. They may reach a point where they are exhausted, frustrated, or even angry because, despite their best efforts, they may not get the desired results and may develop health problems related to diabetes despite their hard work.
They feel overwhelmed by the neverending management of diabetes. This upset is diabetes distress.
What is diabetes burnout?
When diabetes distress persists for long enough, your loved one may slip into unhealthy habits, even after years of good management. Habits like no longer checking their blood sugar, avoiding appointments, making frequent unhealthy food choices, and having no motivation to make changes. This is diabetes burnout.
How are these different from depression?
Diabetes distress and burnout are acute and transient. In other words, they come and go, are usually short-lived, and can be somewhat difficult to resolve. Depression is chronic, persisting for long periods, or constantly recurring, and is hard to resolve. People with diabetes are two to three times more likely to experience depression than those without diabetes.
Diabetes distress and burnout are typically situational. They often come on when a person with diabetes is experiencing unrelated stress, like a major home repair, financial setback, an injury, or family problems. It is during these times of additional stress that diabetes management becomes especially inconvenient and frustrating. As the situation resolves, distress and burnout frequently follow suit.
Depression, however, sets in and remains over time. While we often attempt to attribute depression to a situation (death of a loved one, moving out of the home, chronic disease diagnosis), we know that depression is a more complex condition that has no single cause. Depression does not seem to resolve when situational stress decreases or with time and distance from the events thought to cause it.
There are also various types of depression, based on duration, intensity, and level of disruption to daily functions.
Diabetes distress and burnout are very real and need to be addressed, though they are not considered medical illnesses. Depression, on the other hand, is a medical illness that affects how your loved one feels, the way they think, and how they act. Not just about one aspect of their lives at any given time, but rather all aspects of their lives at all times.
Depression is considered a medical illness because known chemical changes are occurring in the brain and body that create feelings of despair, drive loss of interest, and disrupt important daily functions like sleep, appetite, and mental processes. This creates a cycle that persists until it is broken. People can't simply decide to "snap out of it."
Can both be present?
Absolutely. Diabetes distress or burnout can be layered onto existing depression. This is why it is so important to seek support from a qualified mental health professional. A licensed therapist can help your loved ones cope with distress and burnout, and understand symptoms of depression. There are many factors that contribute to distress, burnout, and depression. Therapists at Helpful utilize a relational and evidence-based approach, collaborating with clients on a tailored treatment plan so that clients can feel more empowered to not just cope, but thrive. Learn more about our therapists and sign up for a free consultation here.
RESOURCES
Association of Diabetes Care & Education Specialists (ADCES)
American Psychiatric Association
Diabetes UK. (n.d.). What is diabetes distress and burnout? Link
Kiriella, D.A., Islam, S., Oridota, O., Sohler, N., Dessenne, C., de Beaufort, C., et al. (2021). Unraveling the concepts of distress, burnout, and depression in type 1 diabetes: A scoping review. eClinicalMedicine, 2021 Oct, 40, 101118. doi: 10.1016/j.eclinm.2021.101118
National Institute of Mental Health
U.S. Centers for Disease Control and Prevention
No content in this app, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.
Get more support and guidance on insurance benefits, medical records and legal forms.
Helpful brings together your insurance benefits, legal documents, and medical records in one personalized place — so you always know what you have, and never have to search again.
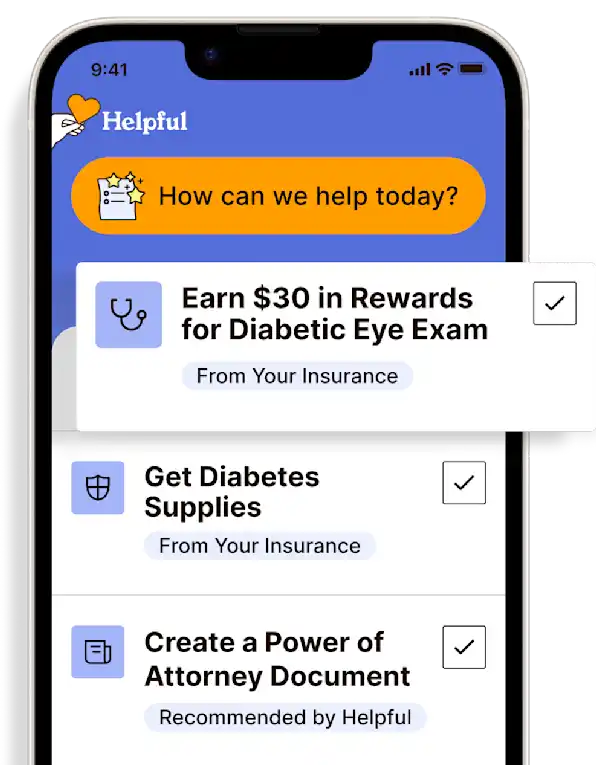
Technology for Health Tasks. Mental Health for the Tough Stuff.
Helpful connects your medical records, insurance, and caregiving tasks automatically. And when you need more than logistics, a therapist is here to guide you.
In-Network and Covered
For Individuals, Couples and Families
HIPAA Compliant, Data Stays Private
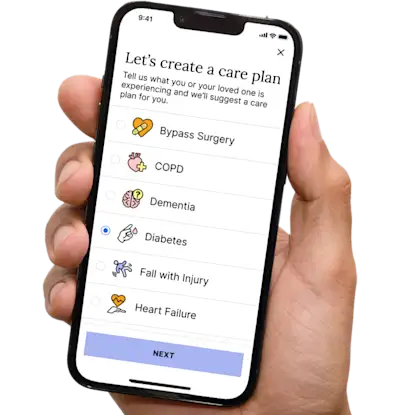

Healthcare Tasks Simplified

From syncing records to spotting drug interactions, Helpful does the heavy lifting, turning complex health info into clear tasks and showing you benefits you can actually use, giving you clarity and control over your care.

In-Network Mental Health

Our licensed therapists are here to support you and your loved ones through stress, burnout, and life’s hardest moments, with an inclusive, compassionate approach that works with most insurance plans.

Create Legal Documents

Plan ahead by creating will, trusts, advance directives and more, that ensure your wishes are honored in the event you can’t speak for yourself -with Helpful guiding you every step of the way.